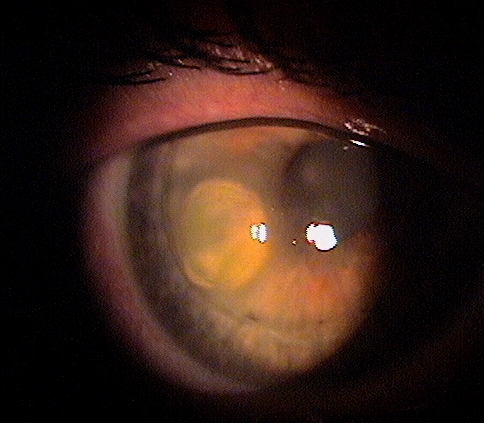
We continued moxifloxacin (Vigamox) BID OD for infection prophylaxis and initiated therapy with cyclosporine 0.05% (Restasis) BID OD and doxycycline 100 mg PO daily for their anti-inflammatory effects. A formal consultation was made with rheumatology. She had never seen a rheumatologist.īlood work for associated systemic conditions was drawn including complete blood count (CBC), blood urea nitrogen (BUN), creatinine, erythrocyte sedimentation rate (ESR), rheumatoid factor (RF), antinuclear antibodies (ANA), antineutrophil cytoplasmic antibodies (ANCA), anti-Ro and anti-La antibodies, and angiotensin-converting enzyme (ACE). We contacted her primary care physician who stated she had "polyarteritis" diagnosed 5 years ago that was "rheumatoid factor negative." In addition to the chronic daily oral prednisone, she was supposed to be taking methotrexate 20 mg every 4 weeks, but regularly missed her appointments for the injections. The anterior chamber cell and flare was believed to be reactive inflammation secondary to the corneal process. The presentation was most consistent with peripheral ulcerative keratitis (PUK) with corneal melt resulting in prominent corneal thinning. The patient presented to the University of Iowa Hospitals and Clinics (UIHC) with a peripheral corneal ulceration in the right eye in the setting of arthritis and an unclear history of rheumatologic disease. The fluorescein stain (C) more clearly reveals the area of epithelial defect. There is adjacent conjunctival injection.

Review of SystemsĬomplete review of systems is negative except as in HPI. There is no history of tobacco or illicit drug use. Oral Prednisone 60 mg daily for the past 12 days, furosemide, metoprolol Social History Moxifloxacin (Vigamox) twice daily, OD Systemic medications Hypertension, possible "rheumatoid arthritis," dementia Ocular medications No family history of rheumatologic or significant ocular disease.

History of cataract extraction in both eyes 3 years ago. This was increased to 60mg PO daily by her local ophthalmologist about 2 weeks prior to her referral. She was a poor historian but apparently carried a diagnosis of "rheumatoid arthritis" for which she chronically took 5 mg of oral (PO) prednisone daily. The patient was treated with prednisolone acetate 1% drops every 2 hours in the right eye locally, but this was discontinued as corneal thinning was noted. Since that time, she had experienced pain, tearing, photophobia, and decreased vision in the eye. She began experiencing foreign body sensation in the right eye about 2 months prior to presentation after getting poked in the eye while gardening. A 79-year-old woman was referred for the evaluation of a corneal ulcer in the right eye (OD).
